 |
 |
- Search
| Ann Geriatr Med Res > Volume 25(3); 2021 > Article |
|
Abstract
Background
Pain is one of the most critical issues in older adults, and the place of residence may play an important role in pain characteristics and related factors. However, it is an understudied subject. This study investigated differences in pain characteristics and functional associations between nursing home residents and community-dwelling older adults.
Methods
Older adult participants were recruited from nursing homes (n=73) and the community (n=73). Pain characteristics, including type, intensity, and number of pain sites, were evaluated. Other outcome measures were functional mobility, walking speed, functional independence, physical activity, anxiety, depression, and health-related quality of life.
Results
Nursing home residents experienced musculoskeletal pain more frequently and had a greater number of pain sites than community-dwelling older adults (p<0.05). Walking speed and mobility were significantly lower and anxiety and depression were significantly higher in nursing home residents (p<0.05). While higher pain intensity was significantly correlated with low scores on physical measures, low health-related quality of life, and higher depression and anxiety symptoms in both groups (p<0.05), the magnitudes of the correlations were much higher in nursing home residents. The number of pain sites was significantly correlated with low scores on physical measures, low health-related quality of life, and higher depression and anxiety symptoms mainly in nursing home residents (p<0.05).
Conclusion
Compared to community-dwelling older adults, nursing home residents experienced musculoskeletal pain more frequently and at more sites in the body. Higher pain intensity and number of pain sites were associated with worse clinical variables, mainly in nursing home residents. This study highlights the importance of regular pain assessment, especially in nursing home care settings.
With decreased birth rates and improved life expectancy, the older population has increased accordingly. For multiple reasons, many older adults prefer staying at home to living in a nursing home. Therefore, determining the risk factors presented in nursing homes is important not only for older adults but also for their families, clinicians, researchers, and policymakers. Pain is an important outcome measure in the geriatric field because it can influence many aspects of physical, emotional, and social functions. For example, studies have shown significant associations between pain and depression, anxiety, social isolation, sleep and cognitive disorders, delirium, impaired activities of daily living, increased utilization of healthcare services, nursing home residence, and, consequently, lower quality of life.1,2)
Several individual characteristics, such as care setting, can influence the prevalence of pain; therefore, pain prevalence in older adults may vary according to the place of residence.1) The prevalence of significant pain problems is 25%ŌĆō50% in community-dwelling older adults and 45%ŌĆō80% in nursing home residents.3) Pain leads to higher healthcare costs in older adults; therefore, improving pain management should be an important goal for healthcare services, especially in long-term care settings such as nursing homes.1) However, pain management is often inadequate among older adults and is a significant problem in home healthcare.2).
The prevalence of neuropathic pain is generally considered to be underestimated in older adults.4) Moreover, the prevalence of neuropathic pain is likely to increase soon because the population is ageing and the survival rates of people with diseases associated with neuropathic pain are increasing.4) However, studies on the influence of neuropathic pain on older adult functioning are scarce and have inconsistent results.5) In addition, most such studies mainly focused on specific conditions such as diabetic peripheral neuropathy and postherpetic neuralgia. Musculoskeletal pain is a common problem in older adults and often leads to their decreased functional ability and quality of life.6) Since neuropathic and musculoskeletal pain have different characteristics and treatment methods, determining their prevalence and impact is essential.7) However, there is less precise information about the types of pain and pain-related factors among nursing homes or community-dwelling older adults, which is important for designing targeted prevention and intervention programs. Thus, the current study investigated the pain characteristics and associated factors in nursing home residents and community-dwelling older adults.
This cross-sectional study was approved by the Ethics Review Board of Near East University (IRB No. 2019/65-716, date: 22.01.2019) and performed in accordance with the ethical standards in the Declaration of Helsinki. Before study commencement, all participants provided written informed consent.
The convenience sampling method was used to recruit participants from four different nursing homes located in Gazimagusa and Lefkosa, as well as community-dwelling older adults from Gazimagusa and surrounding villages in Turkish Republic of Northern Cyprus. A researcher from the study visited these nursing homes and explained the aims and scope of the study to older adults during their collective activities such as breakfast and lunch. Individuals who volunteered to participate in the study were screened according to the inclusion and exclusion criteria. The tests and questionnaires were then administered to the eligible participants. For the recruitment of community-dwelling people, brochures about the study were distributed to local residents, and posters were attached to places that were likely to grab attention. Older adults who were interested in this study were then evaluated.
The inclusion criteria were age >65 years, ability to walk outdoors, and independence in activities of daily living. Participants who were living in their homes were classified as community-dwelling adults, while those living in a nursing home were classified as nursing home residents. Participants with uncontrolled diabetes and hypertension, severe vision and hearing loss, and a Mini-Mental State Examination score of <22 for educated or <18 for uneducated older adults were excluded.8)
A systematic review reported the frequencies of pain in older people varying between 49% and 83%.9) Based on pain frequencies of 49% and 83% in each of the two groups, the required study sample size was calculated to be 144 for a power of 99% and 95% confidence level using Open Source Epidemiologic Statistics for Public Health (OpenEpi) version 3.01 (http://www.openepi.com).
Musculoskeletal pain results from the activation of nociceptors that innervate ligaments, small joints, muscles, and tendons, whereas neuropathic pain results from a lesion or dysfunction of the peripheral or central nervous systems.10) The painDETECT questionnaire can be used to distinguish between these two types of pain.10) The maximum and minimum possible scores of the painDETECT questionnaire were 38 and ŌĆō1, respectively. Scores Ōēż12 indicate a non-neuropathic component (i.e., musculoskeletal pain), while scores Ōēź19 indicate a neuropathic component (i.e., neuropathic pain).10,11) Even though the results are uncertain between these thresholds, a neuropathic pain component may be present.10,11) Therefore, we categorized these uncertain results as neuropathic pain.11) This study used the Turkish version of the painDETECT questionnaire, which demonstrated good psychometric properties.11) The frequencies of pain in different body regions were determined using the Nordic Musculoskeletal Questionnaire, which assessed the presence of pain within the last year and week among the nine different body parts.12,13) The Turkish version of the Nordic Musculoskeletal Questionnaire is reliable and valid, with excellent internal consistency and moderate to almost perfect test-retest reliability.12) The current pain intensity was evaluated using a visual analog scale.
The Timed Up and Go (TUG) test was used to assess mobility, static balance, and dynamic balance.14) The TUG test has good psychometric properties in community-dwelling older adults15) and frail older adults referred to a hospital.16) The participants were asked to sit in a chair, walk 3 m away, turn, walk back to the chair, and sit down. The score was recorded in seconds, with higher scores indicating decreased mobility.
The 10-m walk test is a valid and reliable measure used to assess walking speed in older people.15,17,18) The participants were asked to walk at a comfortable speed, which was reported in m/s.
Performance in activities of daily living and mobility were assessed using the modified Barthel Index.19) Higher scores on the modified Barthel Index indicate a greater degree of independence.
Physical activity level was assessed using the Turkish version of the Rapid Assessment of Physical Activity (RAPA), a self-reported measure.20,21) The RAPA has two subscales: RAPA-Aerobic and RAPA-Flexibility and Strength. However, only two participants from the community-dwelling group reported that they were performing strength exercises; therefore, we analyzed and reported only the RAPA-aerobic scores.
Symptoms of anxiety and depression were assessed using the Hospital Anxiety and Depression Scale (HADS), which has two subscales. Higher scores indicate higher levels of anxiety and depression for each subscale.22) The internal consistency of the HADS was excellent in the general population aged 65ŌĆō80 years,23) and its Turkish version is valid and reliable.24)
Health-related quality of life was measured with the Short Form-36 Health Survey (SF-36), which measures eight health-related quality of life domains.25) We reported the sum scores of the physical and mental components, with higher scores indicating higher levels of quality of life. The SF-36 has stronger evidence of reliability and validity than other generic health-related quality of life instruments in older adults in different settings,26) and its Turkish version is psychometrically sound.27)
Kolmogorov-Smirnov test results and histograms were used to assess the data distributions, which were mostly non-normal. Therefore, Mann-Whitney U tests were conducted to compare the differences between the study groups (community-dwelling older adults vs. nursing home residents). Categorical variables were compared using chi-squared tests. For correlation analysis, we calculated Spearman rank-order correlation coefficients, which were categorized as strong (>0.5), moderate (0.3ŌĆō0.5), and weak (0.2ŌĆō0.3).28) The Holm-Bonferroni sequential correction method was used to correct for type 1 errors due to multiple correlations. Statistical significance was set at p<0.05. The IBM SPSS Statistics for Windows, version 25.0 (IBM Corp., Armonk, NY, USA) was used to perform the statistical analyses.
The participants in this study included 73 community-dwelling residents and 73 nursing home residents. Age, sex, and body mass index did not differ significantly between the two groups (p>0.05) (Table 1). The frequency of musculoskeletal pain and the number of pain sites in the last year and week as well as the TUG, HADS-anxiety, and HADS-depression scores were significantly higher in nursing home residents (p<0.05). The modified Barthel Index, walking speed, and RAPA were significantly lower in nursing home residents (p<0.001). We observed no significant differences in SF-36 scores between the two groups (p>0.05). Table 1 presents the results of the comparisons of the participantsŌĆÖ pain characteristics, physical functions, anxiety, depression, and quality of life.
The nursing home residents reported significantly higher frequency of musculoskeletal pain in the hips/thighs, knees, and ankles/feet regions in the last year and week (p<0.05) (Fig. 1). Moreover, they reported significantly higher frequency of neuropathic pain in the last year in the upper back, lower back, knees, and ankles/feet regions (p<0.05). In addition to these regions, they reported significantly higher frequency of neuropathic pain in the hips/thighs in the last week (Fig. 2). In contrast, community-dwelling older adults reported significantly higher frequency of neuropathic pain in the wrist/hand region in the last year and week (p<0.05) (Fig. 2).
Regardless of the type of pain, the nursing home residents reported significantly higher frequency of upper back, hips/thighs, knees, and ankles/feet pain in the last year and week (p<0.05). In contrast, community-dwelling older adults reported significantly more wrist/hand pain in the last year and week (p<0.05). Fig. 3 shows the distribution of pain sites during the previous year and week.
Table 2 presents the correlations between current pain intensity and the number of pain sites during the last year and week as well as other study measures. Current pain intensity was significantly related to all study variables in community-dwelling older adults (p<0.05). Current pain intensity was also significantly related to all study variables, except for the physical activity class (p=0.435) in nursing home residents. The correlations were much stronger in nursing home residents. The number of pain sites in the last year was not significantly correlated with any study outcome measures in the community-dwelling older adults (p>0.05) but was significantly correlated with all study measures (p<0.05) except for the RAPA (p>0.05) in nursing home residents. The number of pain sites in the last year was significantly correlated with the TUG, SF-36-physical and mental components in community-dwelling older adults (p<0.05) and with all study measures (p<0.05), except for the RAPA (p>0.05) in the nursing home residents.
This study investigated pain characteristics and related factors among nursing home residents and community-dwelling older adults. We observed a significantly higher frequency of musculoskeletal pain in nursing home residents; however, pain intensity did not differ significantly between nursing home residents and community-dwelling older adults. In addition, nursing home residents had a greater number of pain sites than community-dwelling older adults. While pain intensity and the number of pain sites were significantly associated with physical function, independence level, depression, anxiety, and quality of life in both nursing home residents and community-dwelling older adults, these associations were stronger among nursing home residents.
The frequency of pain in older people can vary according to the place of residence. Studies have indicated that the prevalence of pain ranges from 25% to 50% in community-dwelling older adults and from 45% to 80% in nursing home residents.3) However, all participants experienced pain regardless of their place of residence. Our results showed a significantly higher frequency of musculoskeletal pain in nursing home residents (67.1%) than in community-dwelling older adults (42.5%). A large, multicenter study reported a 52.5% prevalence of neuropathic pain in older people presenting to outpatient clinics in Turkey.29) However, a population-based study of 5,326 older adults reported prevalences of neuropathic and musculoskeletal pain of 13.7% and 30%, respectively.30) Various factors, such as pain definitions and recall periods, can be related to inconsistency in pain prevalence in different studies.
In our study, regardless of the type of pain, nursing home residents reported more upper back, hips/thighs, knees, and ankles/feet pain in the last year and week than community-dwelling older adults. In contrast, community-dwelling older adults reported more wrist/hand pain in the previous year and week. The upper limbs are used in many daily living activities, from performing the simplest tasks related to self-care, which involves the basic activities of daily living, to the most complex, such as instrumental activities of daily living mainly related to independence in the management of family life, use of domestic appliances, personal or public transport, and control of their medication and finance.31) In addition, upper limb function tends to decrease with age in older people.32) We speculate that since community-dwelling older adults perform these upper limb-related activities of daily living more often than nursing home residents, overuse disorders such as entrapment neuropathies occur more commonly in this population. This might explain the higher frequency of neuropathic pain and wrist/hand region involvement in community-dwelling older adults. However, we did not investigate the origin of pain, although the frequency of neuropathic pain was usually higher in nursing home residents than in community-dwelling older adults. Therefore, further research is required to confirm our results. A detailed assessment of pain distribution according to the body regions identified in our study may help rehabilitation professionals to design preventive rehabilitation programs targeting pain in older people. In this process, it would be reasonable to target different body regions according to the place of residence.
The number of pain sites was also a notable risk factor for physical dysfunction. For example, multiple pain sites were associated with fall risk in older adults.33) Moreover, the number of joint pain sites was associated with incident mobility disability in older adults34,35) and was a better predictor of disability measures than pain intensity and interference with activities.36) Musculoskeletal pain was also associated with mobility disability, walking speed, depressive symptoms, body mass index, and physical activity in community-dwelling older adults.34,35) Similarly, we found that the number of pain sites was associated with low physical measure scores among nursing home residents. These residents had a significantly greater number of pain sites, which were associated with worse physical function, depression, anxiety, and health-related quality of life.
Functional limitations and depression are common complaints in older adults and, when accompanied by pain, may significantly impact daily life.37) A recent study showed that pain was significantly associated with physical frailty, as determined by exhaustion, slowness, weakness, low physical activity, and weight loss, in community-dwelling older adults.38) Another study showed that pain was associated with functional limitations, fatigue, sleeping problems, depressed mood, and quality of life.37) However, previous research was conducted on the general older population and little is known about the differences between nursing home residents and community-dwelling older adults. Our results indicated that higher current pain intensity was correlated with slower walking speed, mobility, functional independence, and quality of life in nursing home residents and community-dwelling older adults. Higher current pain intensity was also correlated with higher anxiety and depression in both groups, with much stronger correlations observed among nursing home residents.
Previous studies have suggested that nursing home residents believed their pain to be intractable and often did not complain to staff.39) Our results showing the close association of pain with poor quality of life, physical dysfunction, and high depression and anxiety in nursing home residents suggests that pain must be assessed regularly, even in the absence of a complaint by an older adult. In this context, regular rehabilitation programs targeting pain management and prevention should be implemented in nursing home settings. In addition, pharmacological treatment options should be evaluated. Longitudinal studies are also needed to investigate the most effective pain treatment options and their effects on quality of life, physical function, depression, and anxiety in older adults, especially those living in nursing homes.
Our results suggest the importance of pain assessment to guarantee the health of older adults by demonstrating the high prevalence of pain and the factors associated with pain. In addition, the factors associated with pain differed between nursing home residents and community-dwelling older adults. Pain assessment should aim to characterize the pain type and physical, emotional, functional, and social impairments associated with pain in older adults based on the place of residence.
Our results may have clinical implications. Our finding that nursing home residents were significantly more affected by pain than community-dwelling older adults highlights the importance of including regular pain assessment and management programs in nursing home care settings, even in the absence of complaints by older adults. The musculoskeletal pain sites observed in this study might guide clinicians and researchers in planning rehabilitation programs targeting musculoskeletal pain. However, due to the cross-sectional design of our study, we cannot conclude that the associated factors will decrease when pain decreases. Studies investigating the effects of pain management programs on these associated factors are needed. While we observed no significant difference in pain intensity between the nursing home residents and community-dwelling older adults, less pain intensity was significantly associated with physical function, independence, anxiety, depression, and quality of life in nursing home residents. Therefore, clinicians should consider the patientŌĆÖs place of residence.
Our study has several limitations. First, we did not investigate the origin of pain. Disease-specific pain might have different effects on the variables assessed in our study. Moreover, the types and severity of diseases that cause musculoskeletal and neuropathic pain require further investigation. Second, we accepted pain in a broad context and did not differentiate between acute and chronic pain. Third, we included only older adults without significant cognitive impairment. However, cognitively impaired older adults tend to have communication problems and cannot report pain properly; thus, their pain is under-detected.40) Therefore, our results cannot be generalized to such individuals. Fourth, owing to its cross-sectional design, our study can only reveal associations and cannot infer causality or provide an explanatory clarification for such associations. Finally, the sample size was small and our results are prone to significant bias due to the convenience sampling method. Therefore, longitudinal studies with large sample sizes and more robust sampling methods are needed to draw definitive conclusions.
In conclusion, the frequency of musculoskeletal pain was significantly higher in nursing home residents, whereas that for neuropathic pain was higher in community-dwelling older adults. While current pain intensity was associated with walking speed, mobility, functional independence level, anxiety, depression, and quality of life in both nursing home residents and community-dwelling older adults, these associations were much stronger in nursing home residents. A higher number of pain sites during the last year and week was significantly associated with lower walking speed, mobility, independence level, health-related quality of life, and more anxiety and depression symptoms in older adults living in nursing homes, while only the number of pain sites during the last week, mobility, and health-related quality of life in were significantly associated in community-dwelling older adults. The number of pain sites during the last year was not associated with any study variables in community-dwelling older adults. The results of this study highlight the importance of including regular pain assessment in nursing home care settings, even in the absence of complaints by older adults.
Fig.┬Ā1.
Distribution of pain sites according to the place of residence in the last year (A) and week (B) in people with musculoskeletal pain (n=66). Values are presented as percent. *Statistically significant difference.
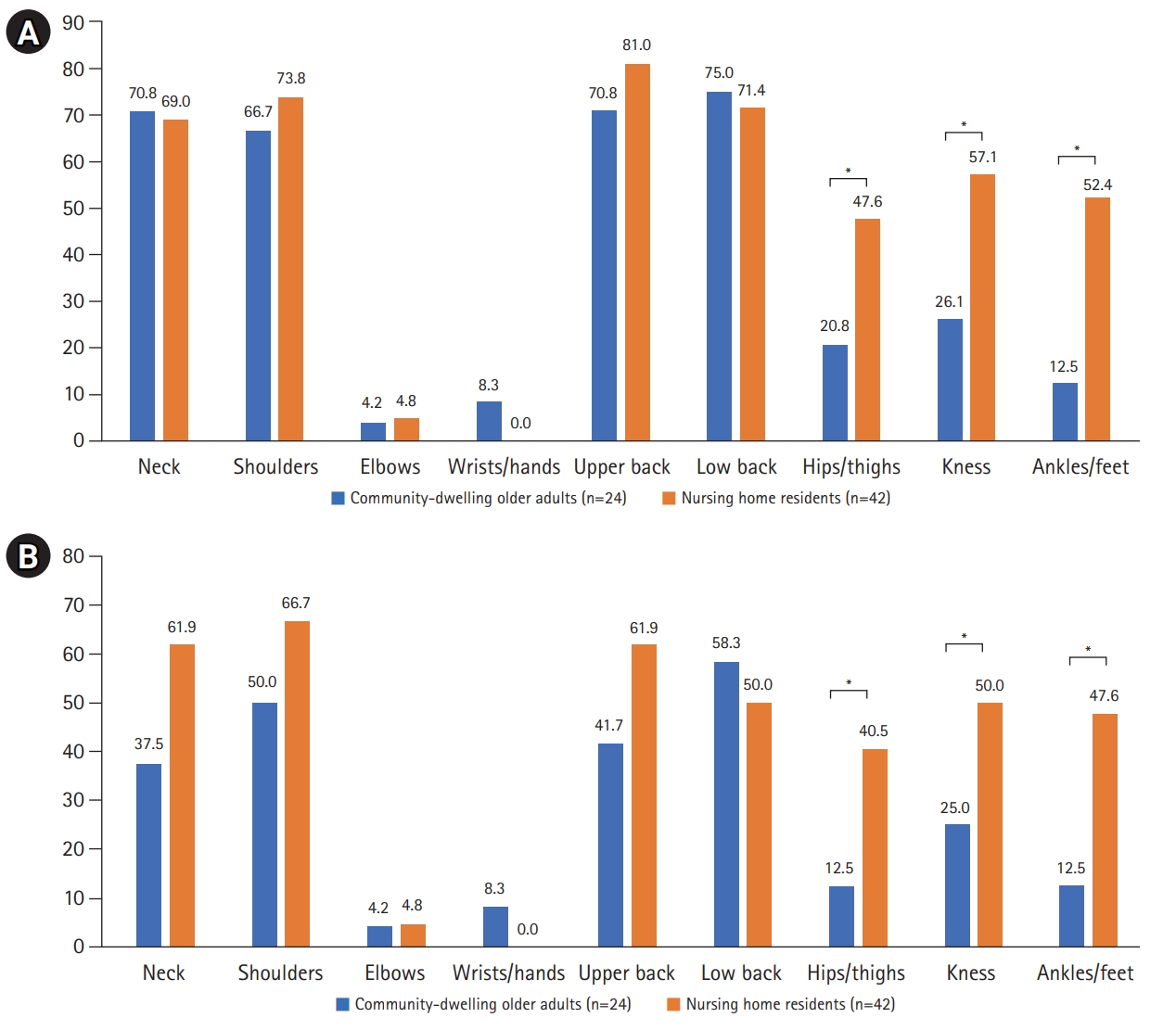
Fig.┬Ā2.
Distribution of pain sites according to the place of residence in the last year (A) and week (B) in people with neuropathic pain (n=80). Values are presented as percent. *Statistically significant difference.
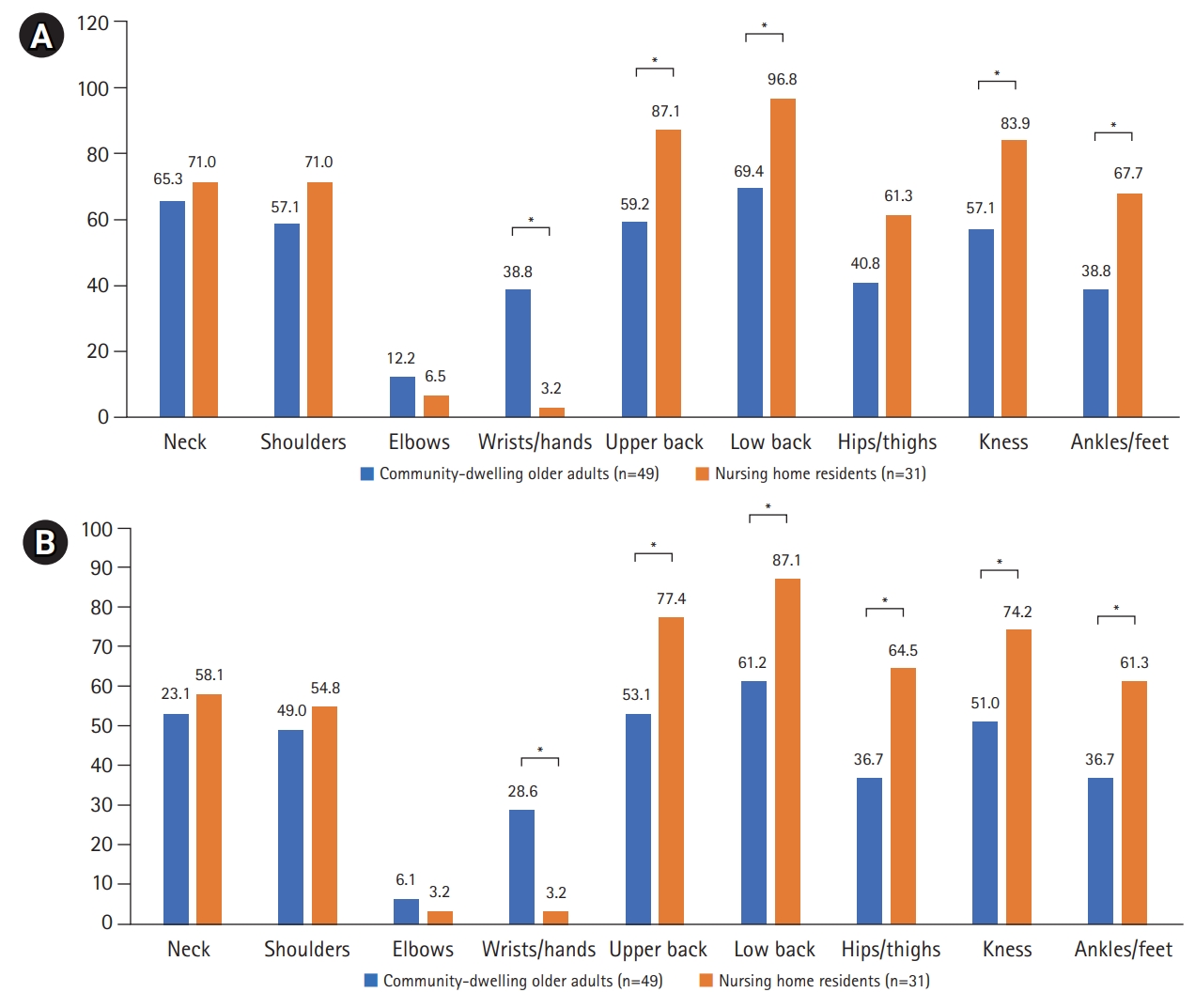
Fig.┬Ā3.
Distribution of pain sites according to the place of residence in the last year (A) and week (B) in the whole sample (n=146). Values are presented as percent. *Statistically significant difference.

Table┬Ā1.
Comparisons of participant demographic and pain characteristics, physical functions, anxiety, depression, and quality of life
| Variable | Community-dwelling older adults (n=73) | Nursing home residents (n=73) | p-value |
|---|---|---|---|
| Age (y) | 73.5┬▒6.9 | 75.9┬▒8.1 | 0.094 |
| Sex, female | 34 (46.6) | 27 (37.0) | 0.240 |
| Body mass index (kg/m2) | 27.44┬▒3.80 | 27.43┬▒4.19 | 0.693 |
| Type of pain | 0.003* | ||
| ŌĆāMusculoskeletal | 24 (32.9) | 42 (57.5) | |
| ŌĆāNeuropathic | 49 (67.1) | 31 (42.5) | |
| Current pain intensity (cm) | 5.4┬▒1.4 | 5.2┬▒1.5 | 0.470 |
| Number of pain sites during the last 12 months | 4.1┬▒1.8 | 5.0┬▒1.5 | 0.002* |
| Number of pain sites during the last 7 days | 3.3┬▒1.9 | 4.3┬▒1.5 | 0.001* |
| Walking speed (m/s) | 0.9┬▒0.2 | 0.7┬▒0.2 | <0.001* |
| TUG (s) | 13.3┬▒3.5 | 16.4┬▒5.2 | <0.001* |
| MBI | 99.1┬▒3.6 | 93.1┬▒11.7 | <0.001* |
| RAPA | 2.9┬▒0.5 | 1.4┬▒0.8 | <0.001* |
| HADS-anxiety | 6.8┬▒3.8 | 9.3┬▒3.6 | <0.001* |
| HADS-depression | 5.8┬▒3.8 | 9.1┬▒3.5 | <0.001* |
| SF-36 physical component | 52.1┬▒21.1 | 50.5┬▒21.6 | 0.620 |
| SF-36 mental component | 57.2┬▒19.3 | 53.7┬▒18.1 | 0.243 |
Table┬Ā2.
Correlations between the number of pain sites during the last year and week and other study measures
| Variable |
Current pain intensity |
Number of pain sites during the last year |
Number of pain sites during the last week |
|||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Community-dwelling older adults (n=73) |
Nursing home residents (n=73) |
Community-dwelling older adults (n=73) |
Nursing home residents (n=73) |
Community-dwelling older adults (n=73) |
Nursing home residents (n=73) |
|||||||
| rho | p-value | rho | p-value | rho | p-value | rho | p-value | rho | p-value | rho | p-value | |
| Walking speed | -0.568 | <0.001* | -0.720 | <0.001* | -0.287 | 0.088 | -0.607 | <0.001* | -0.206 | 0.945 | -0.573 | <0.001* |
| TUG | 0.650 | <0.001* | 0.739 | <0.001* | 0.316 | 0.056 | 0.616 | <0.001* | 0.339 | 0.018* | 0.534 | <0.001* |
| MBI | -0.324 | 0.016* | -0.687 | <0.001* | -0.062 | >0.999 | -0.520 | <0.001* | -0.119 | 0.320 | -0.448 | <0.001* |
| RAPA | -0.336 | 0.016* | -0.093 | 0.435 | -0.088 | >0.999 | -0.140 | 0.237 | -0.108 | 0.945 | -0.205 | 0.081 |
| HADS-anxiety | 0.309 | 0.016* | 0.646 | <0.001* | 0.127 | >0.999 | 0.566 | <0.001* | 0.259 | 0.135 | 0.376 | 0.003* |
| HADS-depression | 0.292 | 0.016* | 0.643 | <0.001* | 0.039 | >0.999 | 0.518 | <0.001* | 0.092 | 0.945 | 0.331 | 0.008* |
| SF-36 physical component | -0.577 | <0.001* | -0.845 | <0.001* | -0.299 | 0.077 | -0.606 | <0.001* | -0.479 | <0.001* | -0.522 | <0.001* |
| SF-36 mental component | -0.412 | <0.001* | -0.794 | <0.001* | -0.238 | 0.220 | -0.579 | <0.001* | -0.373 | 0.007* | -0.471 | <0.001* |
REFERENCES
1. Xu Y, Jiang N, Wang Y, Zhang Q, Chen L, Ma S. Pain perception of older adults in nursing home and home care settings: evidence from China. BMC Geriatr 2018;18:152.



2. Beissner K, Bach E, Murtaugh C, Parker SJ, Trachtenberg M, Reid MC. Implementing a cognitive-behavioral pain self-management program in home health care, part 1: program adaptation. J Geriatr Phys Ther 2013;36:123ŌĆō9.



3. AGS Panel on Persistent Pain in Older Persons. The management of persistent pain in older persons. J Am Geriatr Soc 2002;50(6 Suppl):S205ŌĆō24.

4. McDermott AM, Toelle TR, Rowbotham DJ, Schaefer CP, Dukes EM. The burden of neuropathic pain: results from a cross-sectional survey. Eur J Pain 2006;10:127ŌĆō35.


5. Stompor M, Grodzicki T, Stompor T, Wordliczek J, Dubiel M, Kurowska I. Prevalence of chronic pain, particularly with neuropathic component, and its effect on overall functioning of elderly patients. Med Sci Monit 2019;25:2695ŌĆō701.



6. Podichetty VK, Mazanec DJ, Biscup RS. Chronic non-malignant musculoskeletal pain in older adults: clinical issues and opioid intervention. Postgrad Med J 2003;79:627ŌĆō33.



7. Galluzzi KE. Managing neuropathic pain. J Am Osteopath Assoc 2007;107(10 Suppl 6):ES39ŌĆō48.
8. Keskinoglu P, Ucku R, Yener G, Yaka E, Kurt P, Tunca Z. Reliability and validity of revised Turkish version of Mini Mental State Examination (rMMSE-T) in community-dwelling educated and uneducated elderly. Int J Geriatr Psychiatry 2009;24:1242ŌĆō50.


9. Fox PL, Raina P, Jadad AR. Prevalence and treatment of pain in older adults in nursing homes and other long-term care institutions: a systematic review. CMAJ 1999;160:329ŌĆō33.

10. Freynhagen R, Baron R, Gockel U, Tolle TR. painDETECT: a new screening questionnaire to identify neuropathic components in patients with back pain. Curr Med Res Opin 2006;22:1911ŌĆō20.


11. Alkan H, Ardic F, Erdogan C, Sahin F, Sarsan A, Findikoglu G. Turkish version of the painDETECT questionnaire in the assessment of neuropathic pain: a validity and reliability study. Pain Med 2013;14:1933ŌĆō43.


12. Kahraman T, Genc A, Goz E. The Nordic Musculoskeletal Questionnaire: cross-cultural adaptation into Turkish assessing its psychometric properties. Disabil Rehabil 2016;38:2153ŌĆō60.


13. Kuorinka I, Jonsson B, Kilbom A, Vinterberg H, Biering-Sorensen F, Andersson G, et al. Standardised Nordic questionnaires for the analysis of musculoskeletal symptoms. Appl Ergon 1987;18:233ŌĆō7.


14. Yim-Chiplis PK, Talbot LA. Defining and measuring balance in adults. Biol Res Nurs 2000;1:321ŌĆō31.


15. Steffen TM, Hacker TA, Mollinger L. Age- and gender-related test performance in community-dwelling elderly people: Six-Minute Walk Test, Berg Balance Scale, Timed Up & Go Test, and gait speeds. Phys Ther 2002;82:128ŌĆō37.


16. Podsiadlo D, Richardson S. The timed "Up & Go": a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc 1991;39:142ŌĆō8.


17. Bohannon RW. Comfortable and maximum walking speed of adults aged 20-79 years: reference values and determinants. Age Ageing 1997;26:15ŌĆō9.

18. Peters DM, Fritz SL, Krotish DE. Assessing the reliability and validity of a shorter walk test compared with the 10-Meter Walk Test for measurements of gait speed in healthy, older adults. J Geriatr Phys Ther 2013;36:24ŌĆō30.


19. Shah S, Vanclay F, Cooper B. Improving the sensitivity of the Barthel Index for stroke rehabilitation. J Clin Epidemiol 1989;42:703ŌĆō9.


20. Topolski TD, LoGerfo J, Patrick DL, Williams B, Walwick J, Patrick MB. The Rapid Assessment of Physical Activity (RAPA) among older adults. Prev Chronic Dis 2006;3:A118.


21. Cekok FK, Kahraman T, Kalkisim M, Genc A, Keskinoglu P. Cross-cultural adaptation and psychometric study of the Turkish version of the Rapid Assessment of Physical Activity. Geriatr Gerontol Int 2017;17:1837ŌĆō42.


22. Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983;67:361ŌĆō70.


23. Djukanovic I, Carlsson J, Arestedt K. Is the Hospital Anxiety and Depression Scale (HADS) a valid measure in a general population 65-80 years old? A psychometric evaluation study. Health Qual Life Outcomes 2017;15:193.



24. Aydemir O, Guvenir T, Kuey L, Kultur S. Validity and reliability of Turkish version of hospital anxiety and depression scale. Turk Psikiyatri Derg 1997;8:280ŌĆō7.
25. Ware JE Jr, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992;30:473ŌĆō83.


26. Haywood KL, Garratt AM, Fitzpatrick R. Quality of life in older people: a structured review of generic self-assessed health instruments. Qual Life Res 2005;14:1651ŌĆō68.


27. Kocyigit H, Aydemir O, Fisek G, Olmez N, Memis A. K─▒sa Form 36 (KF-36)ŌĆÖn─▒n T├╝rk├¦e versiyonunun g├╝venilirli─¤i ve ge├¦erlili─¤i [Reliability and Validity of the Turkish Version of Short Form-36 (SF-36)]. Ilac ve Tedavi Dergisi 1999;12:102ŌĆō6.
28. Cohen J. Statistical power analysis for the behavioral sciences. Hoboken, NJ: Taylor and Francis; 2013.
29. Kutsal YG, Eyigor S, Dogan A, Zardaut S, Durmus B, Evcik FD, et al. Neuropathic pain in elderly: a multicenter study. Turk J Geriatr 2016;19:9ŌĆō18.
30. Salman Roghani R, Delbari A, Asadi-Lari M, Rashedi V, Lokk J. Neuropathic pain prevalence of older adults in an urban area of Iran: a population-based study. Pain Res Treat 2019;2019:9015695.



31. Vasconcelos Rocha S, Souza Dos Santos S, Carneiro Vasconcelos LR, Alves Dos Santos C. Strength and ability to implement the activities of daily living in elderly resident in rural areas. Colomb Med (Cali) 2016;47:167ŌĆō71.



32. Kahraman T, Cekok FK, Ugut BO, Keskinoglu P, Genc A. One-year change in the physical functioning of older people according to the international classification of functioning domains. J Geriatr Phys Ther 2021;44:E9ŌĆōE17.


33. Leveille SG, Jones RN, Kiely DK, Hausdorff JM, Shmerling RH, Guralnik JM, et al. Chronic musculoskeletal pain and the occurrence of falls in an older population. JAMA 2009;302:2214ŌĆō21.



34. Shah RC, Buchman AS, Boyle PA, Leurgans SE, Wilson RS, Andersson GB, et al. Musculoskeletal pain is associated with incident mobility disability in community-dwelling elders. J Gerontol A Biol Sci Med Sci 2011;66:82ŌĆō8.


35. Manty M, Thinggaard M, Christensen K, Avlund K. Musculoskeletal pain and physical functioning in the oldest old. Eur J Pain 2014;18:522ŌĆō9.


36. Eggermont LH, Leveille SG, Shi L, Kiely DK, Shmerling RH, Jones RN, et al. Pain characteristics associated with the onset of disability in older adults: the maintenance of balance, independent living, intellect, and zest in the Elderly Boston Study. J Am Geriatr Soc 2014;62:1007ŌĆō16.



37. Jakobsson U, Klevsgard R, Westergren A, Hallberg IR. Old people in pain: a comparative study. J Pain Symptom Manage 2003;26:625ŌĆō36.


38. Nakai Y, Makizako H, Kiyama R, Tomioka K, Taniguchi Y, Kubozono T, et al. Association between chronic pain and physical frailty in community-dwelling older adults. Int J Environ Res Public Health 2019;16:1330.










