|
 |
- Search
| Ann Geriatr Med Res > Volume 28(1); 2024 > Article |
|
Abstract
Background
Methods
Results
Fig.┬Ā2.
Table┬Ā1.
| Variable | Total (n=174) |
Cognitive impairment |
p-value | Effect size | |
|---|---|---|---|---|---|
| Yes (n=77) | No (n=97) | ||||
| Demographics | |||||
| ŌĆāAge (y) | 70.4┬▒6.8 | 73.0┬▒7.8 | 68.3┬▒5.0 | <0.001*a) | 0.315 |
| ŌĆāŌĆā65ŌĆō74 | 133 (76.4) | 47 (61.0) | 86 (88.7) | <0.001*b) | 0.323 |
| ŌĆāŌĆā75+ | 41 (23.6) | 30 (39.0) | 11 (11.3) | ||
| ŌĆāSex (female) | 97 (55.7) | 60 (77.9) | 37 (38.1) | <0.001*b) | 0.398 |
| ŌĆāMarital status (married) | 122 (70.1) | 42 (56.8) | 80 (82.5) | <0.001*b) | 0.340 |
| ŌĆāYears of education (Ōēż5) | 21 (12.1) | 21 (28.4) | 0 (0) | <0.001*b) | 0.425 |
| ŌĆāCurrent smoking | 45 (25.9) | 13 (16.9) | 32 (33.0) | 0.016*b) | 0.183 |
| Comorbidities | |||||
| ŌĆāDCCI | 3.8┬▒1.5 | 4.2┬▒1.5 | 3.5┬▒1.3 | 0.001*a) | 0.246 |
| ŌĆāDrug count | 3.8┬▒2.9 | 4.0┬▒2.6 | 3.6┬▒3.1 | 0.100a) | 0.124 |
| ŌĆāPolypharmacy | 57 (32.8) | 28 (38.4) | 29 (29.9) | 0.367b) | 0.068 |
| ŌĆāAnticholinergic burden (Ōēź1) | 58 (33.3) | 35 (45.5) | 23 (23.7) | 0.003*b) | 0.229 |
| Laboratory parameters | |||||
| ŌĆāNeutrophil (<4├Ś10Ōü╣/L) | 82 (47.1) | 42 (54.5) | 40 (41.2) | 0.081b) | 0.132 |
| ŌĆāLymphocyte (<1├Ś10Ōü╣/L) | 61 (35.1) | 32 (41.6) | 29 (29.9) | 0.109b) | 0.121 |
| ŌĆāN/L (Ōēź8) | 31 (17.8) | 12 (15.6) | 19 (19.6) | 0.493b) | 0.052 |
| ŌĆāAnemia (female <12 g/dL, male <13 g/dL) | 47 (27.0) | 22 (28.6) | 25 (25.8) | 0.680b) | 0.031 |
| ŌĆāCRP (>30 mg/L) | 95 (54.6) | 37 (48.7) | 58 (60.4) | 0.124b) | 0.117 |
| ŌĆāD-dimer (Ōēź0.5 mg/L) | 99 (56.9) | 50 (74.6) | 49 (57.6) | 0.029*b) | 0.177 |
| ŌĆāGFR (<60 mL/min) | 48 (27.6) | 23 (29.9) | 25 (25.8) | 0.548b) | 0.046 |
| ŌĆāLDH (>300 U/L) | 68 (39.1) | 32 (45.7) | 36 (44.4) | 0.876b) | 0.013 |
| Hospitalization characteristics | |||||
| ŌĆāICU admission (yes) | 25 (14.4) | 8 (10.4) | 17 (17.5) | 0.183b) | 0.101 |
| ŌĆāDelirium (yes) | 51 (29.3) | 38 (49.4) | 13 (13.4) | <0.001*b) | 0.392 |
| ŌĆāLength of stay (>7 days) | 131 (75.3) | 55 (71.4) | 76 (78.4) | 0.293*b) | 0.080 |
| Follow-up time (mo) | 15.0┬▒3.2 | 15.5┬▒2.8 | 14.5┬▒3.5 | 0.194a) | 0.098 |
| 15 (11ŌĆō20) | 15 (11ŌĆō19) | 15 (12ŌĆō20) | 0.147 | 0.087 | |
Values are presented as mean┬▒stadnard deviation or number (%) or median (minŌĆōmax).
DCCI, Deyo/Charlson Comorbidity Index Score; N/L, neutrophil and lymphocyte ratio; CRP, C-reactive protein; GFR, glomerular filtration rate; LDH, lactate dehydrogenase; ICU, intensive care unit.
Missing data: Education (7), CRP (2), D-dimer (22), and LDH (23).
Effect size: some widely used suggestions about the magnitude of the effect of r and phi 0.10 (small effect), 0.30 (medium effect) and 0.50 (large effect) 39.
Table┬Ā2.
| Variable | Total (n=174) |
Cognitive impairment |
p-value | Effect size | |
|---|---|---|---|---|---|
| Yes (n=77) | No (n=97) | ||||
| Mood status | |||||
| ŌĆāPHQ-2 | 1 (0ŌĆō6) | 2 (0ŌĆō6) | 1 (0ŌĆō6) | 0.065a) | 0.139 |
| ŌĆāPHQ-2 (Ōēź3) | 38 (21.8) | 23 (29.9) | 15 (15.5) | 0.022*b) | 0.173 |
| ŌĆāGAD-2 | 1 (0ŌĆō6) | 1 (0ŌĆō6) | 0 (0ŌĆō6) | 0.003*a) | 0.228 |
| ŌĆāGAD-2 (Ōēź3) | 34 (19.5) | 24 (31.2) | 10 (10.3) | 0.001*b) | 0.261 |
| Cognitive status | |||||
| ŌĆāT-CogS-TR | 21.6┬▒3.3 | 18.7┬▒2.5 | 24.0┬▒1.3 | <0.001*a) | 0.864 |
Values are presented as median (minŌĆōmax) or number (%) or mean┬▒stadnard deviation.
COVID-19, coronavirus disease 2019; PHQ-2, Patient Health Questionnaire-2; GAD-2, Generalized Anxiety Disorder-2; T-CogS-TR, Turkish version of the Telephone Cognitive Screen.
Effect size: some widely used suggestions about the magnitude of the effect of r and phi 0.10 (small effect), 0.30 (medium effect) and 0.50 (large effect) 39.
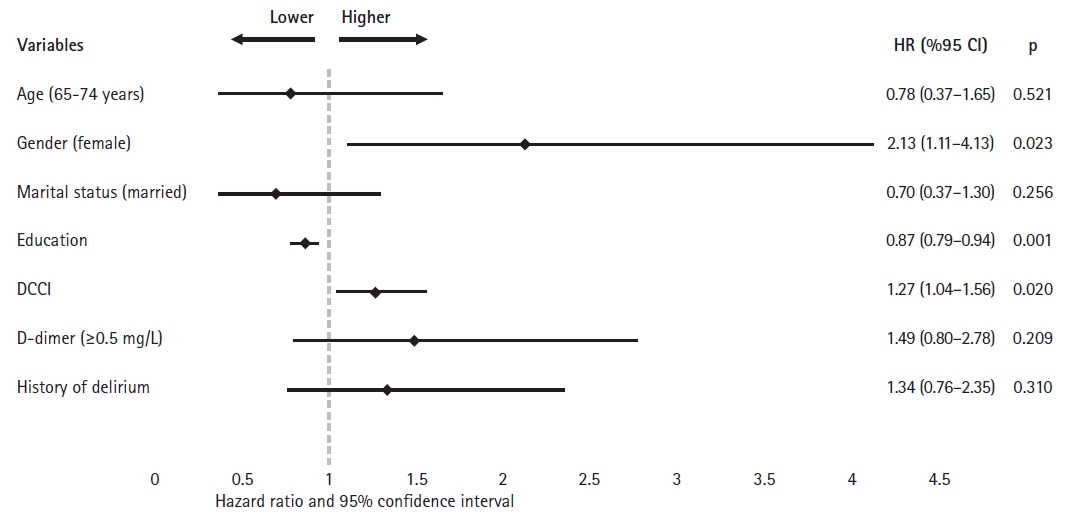
Table┬Ā3.
| Variable |
Univariate |
Multivariate |
||
|---|---|---|---|---|
| HR (95% CI) | p-value | HR (95% CI) | p-value | |
| Age (Ōēź75 y) | 1.98 (1.24ŌĆō3.15) | 0.004* | 0.78 (0.37ŌĆō1.65) | 0.521 |
| Sex (female) | 2.57 (1.50ŌĆō4.41) | 0.001* | 2.13 (1.11ŌĆō4.13) | 0.023* |
| Marital status (married) | 0.47 (0.29ŌĆō0.74) | 0.001* | 0.70 (0.37ŌĆō1.30) | 0.256 |
| Years of education (Ōēż5) | 0.09 (0.02ŌĆō0.37) | 0.001* | 1.45 (0.71ŌĆō2.45) | 0.310 |
| Current smoking | 0.75 (0.41ŌĆō1.38) | 0.357 | - | - |
| DCCI | 1.34 (1.16ŌĆō1.56) | <0.001* | 1.27 (1.04ŌĆō1.56) | 0.020* |
| Anticholinergic burden (Ōēź1) | 1.48 (0.92ŌĆō2.35) | 0.102 | - | - |
| D-dimer (Ōēź0.5 mg/L) | 2.37 (1.33ŌĆō4.23) | 0.003* | 1.49 (0.80ŌĆō2.78) | 0.209 |
| History of delirium (yes) | 1.90 (1.21ŌĆō2.99) | 0.006* | 1.34 (0.76ŌĆō2.35) | 0.310 |