Effects of a Multicomponent Program on Fall Incidence, Fear of Falling, and Quality of Life among Older Adult Nursing Home Residents
Article information
Abstract
Background
Falling is one of the most common problems in older adults and can lead to additional health problems. This study aimed to determine the effects of a multicomponent program on fall incidence and quality of life in older adult nursing home residents.
Methods
This was a quasi-experimental study with a pretest and post-test design. The study population comprised 55 older adults residing in nursing homes. The intervention was a multicomponent program including physical activities, training sessions, and physical environment modifications in nursing homes that was conducted for 8 weeks. The data collection tools included a socio-demographic characteristics form and questionnaires pertaining to the quality of life and fear of falls, which were completed by the participants before and after the intervention.
Results
The mean age of the participants was 68.48 years, and most (90%) were illiterate. We observed a significant difference between the mean number of falls and the scores for fear of falling before and after the intervention (p<0.001). We also observed a significant difference between the total quality of life scores and all of the related dimensions before and after the intervention, indicating that the quality of life of the older adults had improved after the intervention (p<0.001).
Conclusion
The results of this study indicated that the multicomponent fall prevention program was effective in improving the quality of life, fall rate, and fear of falling among older residents in nursing homes. Further studies are needed to explore the long-term effects of these interventions.
INTRODUCTION
Older age is a sensitive period of life that is often associated with disability, decreased physical abilities, and the occurrence of diseases including cardiovascular, respiratory, and muscular diseases as well as other problems. These problems can affect the body’s balance and strength and cause complications such as falls and, subsequently, multiple fractures.1-2)
Twenty to sixty percent of older adults over 65 years of age experience a fall at least once in their lifetime, with half of them experiencing frequent falls. This rate is higher among older adults living in nursing homes.3,4) Approximately one-third of older people living in nursing homes fall at least once a year, with half of them experiencing multiple falls; moreover, approximately 40% of residents aged ≥65 years die as the result of a fall.3,5) The rate of hip fractures in nursing homes is an estimated 1.4/100 person-years.6)
In the European Union, adults over 65 years of age account for half of the deaths caused by unintentional injuries despite representing only 20% of the population.7) Furthermore, in Canada, falls are the most common cause (85%) of injury-related hospital admissions among those aged >65 years.8) In developed countries, fall-related injuries account for 6% of the total medical costs.1) In Iran, 12% of 8,000 hospitalized trauma cases are adults aged 60 years or older, 70% of whom experience falls. The home and the street are the most common sites of falls among older adults in Iran.9)
The estimated rate of mortality among older adults 1 year after a hip fracture ranges between 14% to 36%.6,10) A study in Iran reported that 71% of fall injuries and 76% of hip fractures occurred indoors and that 62% of hip injuries were caused by falls.11)
Falling has serious social and mental consequences, in addition to its economic and physical complications.12) Falling is a serious issue in community-dwelling adults as the resulting psychological consequences may lead to mobility deficits and reduced quality of life.13) This mental injury results from a fear of falling, which cause social isolation in older adults.1)
Many studies have reported a fear of falling as an essential factor for falls.12-14) Moreover, fear of falling is a crucial factor related to reduced life satisfaction and increased nursing home admission rates.3,14) Fear of falling or post-fall syndrome is defined as “an ongoing concern about falling and fall-related dangerous complications”.15) Older adults, because of a fear of falling, refuse many activities such as preparing meals, walking, and activities they have previously performed.16) People with a fear of falling have more mobility limitations and a lower quality of life than do others.12,13,16)
As many risk factors for falling are preventable, fall prevention approaches include determining and assessing fall risk factors, removing and reducing fall risk such as modifying the living environment older adults, teaching and changing the lifestyle of older adults with regular exercise programs, following a proper diet and preventing obesity, controlling medications, living in a calm and stress-free environment, and referring to doctors to assess visual status.17)
Coimbra et al.18) conducted a study on interventions for fall prevention in older people, reporting that fall prevention programs should be multicomponent to effectively reduce the fall risk and rate. Consequently, identification of older adults at risk for falls can minimize fall risk through proper interventions and the design of appropriate programs by individuals and their families and healthcare providers, including nurses, to prevent falls.19) In addition to reduced fall risk in older adults, such programs can prevent fall-related complications such as admission to hospitals and health care centers, physical and psychosocial pressure on older adults and their families, as well as increased economic burdens on families and the society.20,21)
Therefore, given the increasing numbers of older populations and the movement of Iran toward aging, as well as the reported high prevalence of falls among older people and the resulting complications affecting older adults’ health and quality of life, studies on these topics are necessary. Such studies are limited in Iran and most studies utilized a descriptive approach. Because the prevalence rate of falls among older adults in nursing homes is higher than that in adults residing at home,3) this study aimed to determine the effect of a fall prevention program on the fear of falling, fall number, and quality of life among older adults residing in nursing homes.
MATERIALS AND METHODS
Study Design
This study applied a quasi-experimental pretest and post-test design.
Setting and Study Population
The sample comprising 55 eligible older adults was selected from among 103 older adult residents in two nursing homes in the west of Iran. The inclusion criteria were: (1) older people aged 60 years and over; (2) non-frail older adults (based on Edmonton Frail Scale22) score ≤5 points) having the physical ability to perform exercise activities, without medical prohibitions; (3) living for at least 3 months in a nursing home; (4) having fair psychological conditions when entering the study (Abbreviated Mental Test score >7); (5) no severe Alzheimer disease (based on medical diagnosis recorded in adults’ record); (6) willingness to participate in the study; (7) not under simultaneous investigation in other experimental studies; and (8) ability to communicate with others and participate in sessions with or without adjuvant tools (glasses and hearing aids). The exclusion criteria were: (1) unwillingness to maintain study involvement; (2) having an acute physical illness leading hospital admission; and (3) failure to attend training sessions for more than two sessions.
Intervention
The participants’ data were first assessed overall and eligible participants were selected by referring to the center and records. In briefing sessions, the researcher explained the study purpose and work phases to the participants and informed them that the program would last 8 weeks.
The questionnaires were first given to the participants for completion; however, as most of the participants were illiterate, the questions were completed by the researcher with full explanations and in the participants’ native language, with the participants’ consent. To ensure accuracy of the questions related to demographic characteristics, the questionnaire was completed by the researcher after asking individual questions and exploring participant records. The measurements conducted in this study included physical activities, training sessions, and physical environment modifications in nursing homes. Visual training booklets on the correct method of executing the exercises were developed and distributed among the older adults.
The exercise activities involved an initial warm-up that included walking and stretching exercises (5 minutes); strength and balance exercises that included single-limb stance, walking heel-to-toe, clock reaches, single-limb stance with arm, back and side leg raises, wall pushups, and sit-to-stand exercises (10–20 minutes); walking around the grounds of the nursing home and Pilates (10–15 minutes); and cool down (5 minutes), which were performed in the first and second sessions for half an hour, and after improving the adults’ readiness in the subsequent sessions, for 45 minutes in each session. The trainer focused on increasing motivation and exercise adherence among the older adults. In each session, the exercises were revised on the basis of the participants’ ability, and the trainer verified that the diaries were correctly completed. Older adult caregivers in the nursing homes were also provided necessary training to monitor the exercise sessions during the week. The exercises continued three times weekly until the end of the program.
Four training sessions for older adults were carried out once every 2 weeks for 30 minutes to 1 hour in the assembly hall of nursing home centers. The training provided to the older people included education on the causes of falls, the mode of taking medications, environmental risks resulting in falls, and complications that threatened the participants after falling. Fall prevention strategies were then discussed using simple language, images, and objective examples. In addition, two training sessions for center staff (including the center official, occupational therapist, care provider, and nurse assistants) were carried out, regarding the methods for fall risk assessment, fall complications, the impact of medications on falling, and the control of environmental factors affecting falls in older adults.
The physical environment modifications included installing handles next to beds, bathrooms, and toilets; installation of alarm bells in the toilet; installation of fences next to the wall (handrail) in the corridors; replacing burned out and dim light bulbs in rooms and corridors; installation of a small closet next to the bed; removing small rugs in rooms; removing cumbersome objects in rooms, courtyards, and corridors; and other changes to reduce the likelihood of falls in older adults. After the end of the intervention, the participants were followed-up after 4 months by study tools were filled out by them.
Data Collection
The data collection tools comprised four sections. The first section included a demographic questionnaire consisting of items on age, sex, marital status, education level, the number of falls in the past 6 months, and the history of underlying disease. The second section was the Short Form-36 (SF-36) questionnaire that was designed in 1998 by an international organization for quality of life assessment. The SF-36 contains two summary scores—the Mental Component Summary (MCS) and Physical Component Summary (PCS) scores—and the following eight subscales: physical function, bodily pain, role physical, general health, energy/vitality, social function, role emotional, and mental health. Each item is rated on a 5-point Likert scale, ranging from poor to excellent.
The maximum score obtained in each section or subscale ranged from 0 to 100, in which higher scores indicated a better quality of life. The Persian version of the psychometric properties of this instrument was assessed by Montazeri et al.23), who confirmed the reliability and validity of the instrument with Cronbach’s alpha coefficients of 0.77–0.9. The third section was the Falls Efficacy Scale (FES). This instrument is an improved form of the Falls Efficacy Scale International (FES-I) that was the first measure developed to assess the fear of falling and measure individuals’ confidence in performing daily tasks without concern about falling. The FES-I is a self-reported questionnaire consisting of 10 items that assess participants’ level of concern regarding falling when performing 16 daily activities. The FES-I comprises the following items: cleaning the house, getting dressed/undressed, preparing meals, and taking a bath or a shower. Each item of the questionnaire measures the respondent’s concern regarding falling while performing various activities and scores the responses on a 10-point scale ranging from not confident at all to completely confident. The sum of scores ranges from 10 to 100, with higher scores indicating a greater concern about falling. Scores of 50–70 and >70 indicate moderate and high concerns about falling, respectively. This instrument, first described by Tinetti et al.,24) has been developed and validated. Najafi et al.19) assessed the reliability of the instrument with an internal consistency method, with a Cronbach’s alpha coefficient of 0.83.
Ethical Considerations
This study was approved by the Ethics Committee of the Ilam University of Medical Sciences (No. ir.medilam.rec.1396.3). All stages of the research upheld all ethical codes related to the participants, including obtaining informed consent from the adults and their legal proxies, ensuring voluntary participation, maintaining confidentiality and anonymity of participants' identity and the questionnaire responses, and ensuring their right to withdraw from the study at any time.
Statistical Analyses
We performed the statistical analyses using PASW Statistics version 18.0 (SPSS Inc., Chicago, IL, USA) using descriptive statistics (frequency, percent, minimum, maximum, mean, and standard deviation) to describe the variables. We used Kolmogorov–Smirnov tests to assess the normality of the data. Chi-squared tests were used to compare the numbers of falls and risk factors for fear of falling before and after the intervention. Independent t-test, paired t-test, and analysis of variance (ANOVA) were used to calculate the differences in means between groups.
RESULTS
This study excluded two participants who left the nursing home, two who did not attend the training sessions, and one who was hospitalized. Finally, 50 participants consisting of 29 (58%) women and 21 (42%) men were selected and analyzed. The mean age of the participants was 68.48 years, and most (90%) were illiterate. The demographic information of the study participants is shown in Table 1. The mean age, mean residence, and number of falls were higher among those who had a greater fear of falling, with significant differences in the latter two variables (p<0.05).
Table 2 shows the mean falls and fear of falling before and after the intervention, with a statistically significant difference between the mean number of falls and fear of falling before and after the intervention (p<0.001). The number of falls and risk of fear of falling decreased significantly after the intervention compared to those before the intervention (p<0.001).
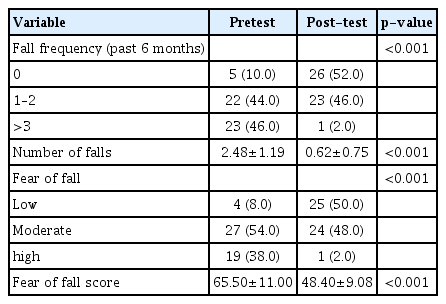
Comparisons of the participants’ frequency of fall and fear of fall before and after the intervention
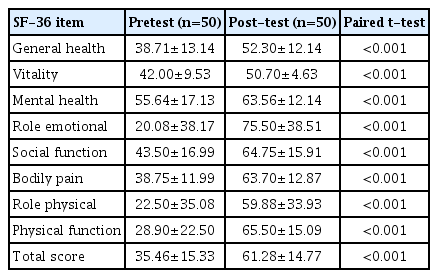
The mean scores of the quality of life and its subscales before and after the intervention are shown in Table 3. We observed a significant difference between the mean score of quality of life in all dimensions before and after the intervention, indicating that the quality of life of the older adults increased after the intervention (p<0.001).
DISCUSSION
This study aimed to determine the effect of a multicomponent fall prevention program on falls, fear of falling, and quality of life among older adults residing in nursing homes. In this study, 90% of the participants had fallen at least once in the 6 months before the intervention. Moreover, those with a long history of residence had a greater fear of falling. Participants with a high risk of fear of falling had experienced more falls during the previous 6 months. Cameron et al.5) reported that 57% of adults living in nursing homes had fallen at least once in the previous 6 months, a finding consistent with our results. The results of a systematic review showed an incidence rate of falls among nursing home residents of 1.7 per adult per year, compared to 0.65 in adults living at home.20) Therefore, falls among nursing home residents are a significant challenge and this population is likely at a higher risk; thus, this issue requires special interventions.
In the present study, the older adults had a lower quality of life before the intervention, in contrast to the quality of life of those living at home reported previously in Iran.25,26) For example, Abdollahi and Mohammadpour26) reported that older adults residing in nursing homes had a lower quality of life in all dimensions of health-related quality of life (HRQOL) than did those living at home. The results of a systematic review showed a direct association between a fear of falling and quality of life in older adults independent of falls experienced.16) In our study, we observed a significant improvement in older adults’ quality of life after the intervention. Moreover, the risk of fear of falling and the number of falls also decreased significantly. Consistent with our results, a study in Finland reported that a multifactorial fall prevention program led to an improvement in the quality of life of older adults.27) In this study, 38% of participants reported a high level of fear of falling. Previous studies have shown that a fear of falling is common among older adults, with prevalences ranging from 3% to 90%, with 50% of those without a fall history showing fear of falling.16,17,28)
The prevention program in the present study included various dimensions such as exercise activities, educational sessions for older adults and staff, and changes in the nursing home environment. Consistent with our findings, Najafi et al.19) showed that fun physical activities acted as a preventive factor in the incidence of balance disorders and falls and that the mean score for fear of falling decreased significantly in the intervention group. Another study in Iran reported that a multicomponent program including environmental modifications and exercise programs resulted in a significant decrease in falls prevalence among older adults living in nursing homes.21) In a systematic review, Granbom et al.29) showed that multicomponent programs are more effective than single-component programs for fall prevention. They also suggested that interventions should integrate the exercise program into daily life and make the home environment safer as the place of residence for older adults to allow older adults to be more likely to continue the exercise program and stay active.
Most of the interventions in fall prevention programs in older people include exercise, use of medication, life environment interventions, use of support technologies such as alarms next to the bed, social environment interventions like training caregivers of older adults, and changes in the organizational system.19-21,29) However, the effects of fall prevention programs on fall risk in older people differ in the literature. For example, a meta-analysis by Vlaeyen et al.30) showed that single-component interventions to prevent falls did not affect the number and risk of falls in more than half of the studies. They also reported that, despite affecting the number of falls and recurrent fallers, the multicomponent fall prevention programs in some studies did not affect the risk of falls. Older adults with disability and cognitive impairment mainly account for nursing home residents. Thus, as the cause of falling in older adults involves various factors, not surprisingly, single-component programs are less useful in preventing falls and their consequences.
The results of this study have many applications for the care of older adults in long-term care centers. Iran will soon be faced with a high volume of older adults, with subsequent dramatic increases in the population living in nursing homes. Regarding the high prevalence of falls and fear of falling in nursing homes, as well as the positive effect of multicomponent fall prevention programs, such programs must be considered as part of routine programs in older adult and primary healthcare centers. Our experiences in conducting this study suggest that staff working in such care centers have inadequate perception and knowledge regarding the principles associated with care for older adults and fall prevention methods. In most cases, caregivers lack specialized education on care for older adults. Thus, continuous education programs on fall prevention and methods for fall risk assessment should be considered for the staff of older adult care centers to better understand this issue and take necessary measures.
Despite its strengths, this study has several limitations. First, as this study was conducted in a western city of Iran, the results may not be generalized to other geographic areas. Second, this study did not use a control group because of executive problems and the lack of nursing homes. Further studies are needed to evaluate the long-term effects of multicomponent programs on fall rate and quality of life in older adults. Finally, it is also necessary to develop programs with a more standard approach, with consideration of the effects of these programs on fall complications, such as fractures and hospitalization, from a cost-effectiveness standpoint.
In conclusion, the results of this study showed that a multicomponent fall prevention program including physical activities, educational sessions for older adults and staff, and changes in the nursing home environment could help improve the quality of life, fall rate, and fear of falling among older adult residents of nursing homes. However, more research is needed to examine the effects of these interventions on fall rate and fall complications among older adults.
Notes
CONFLICT OF INTEREST
The researchers claim no conflicts of interest.
AUTHOR CONTRIBUTION
Conceptualization, AA, MB; Data curation, AA, MB; Funding acquisition, AA, MB; Investigation, AA, MB; Methodology, AA, MB; Project administration, AA, MB; Supervision, AA; Writing-original draft, AA, MB; Writing-review & editing, AA, MB.