Short Physical Performance Battery Cutoff Points Using Clinical Outcomes for At-Risk Older Adults in Singapore: An Exploratory Study
Article information
To the Editor:
The Short Physical Performance Battery (SPPB) is a reliable and valid measure of physical performance that examines three components of lower extremity function: standing balance, gait speed, and repeated sitting-to-standing, with scores ranging from 0 (worst) to 12 (best).1) Poor physical performance based on the SPPB is associated with adverse outcomes such as increased fall risk, functional and cognitive impairment, hospital readmission, and all-cause mortality. The SPPB is an effective screening tool for frailty and sarcopenia2) in older persons, with acceptable sensitivity and specificity.3) Because of the increasing prevalence of frailty and sarcopenia with population aging, automated versions have been developed using modern sensor technologies to facilitate the scalability and widespread use of the SPPB for the assessment of physical performance in community and clinical settings to enable earlier identification and timely interventions in at-risk older adults.4)
Depending on the clinical indication, recommendations differ regarding SPPB cutoff values. The European Working Group on Sarcopenia in Older People 2 recommends a cutoff of ≤8,5) while the Asian Working Group for Sarcopenia 2019 (AWGS-2019) recommends a cutoff of ≤9,6) whereas the cutoff that maximized both sensitivity and specificity for the frailty phenotype was ≤8 points for men and ≤7 for women.2) Moreover, the SPPB may exhibit a ceiling effect, with one study reporting that ≥20% of participants attained the maximum score of 12.7) The ceiling effect is more commonly observed in community studies that include higher functioning and younger participants and less likely in studies involving older adults.2,7,8) Therefore, the reference values for the SPPB are outcome- and population-dependent.
The Yishun Study in Singapore recently recommended an optimal cutoff of ≤11 for both sexes to discriminate sarcopenia in healthy older persons aged ≥60 years. The study limitations suggest caution in the widespread adoption of the higher cutoff, including cutoffs derived based on sarcopenia diagnosis instead of clinically relevant outcomes, healthy community-dwelling participants (mean SPPB score of 11.4 in sarcopenia) with possible spectrum bias, and fair-poor diagnostic performance of the SPPB for sarcopenia (area under the curve [AUC], 0.54–0.64). As this cutoff is much higher than previous cutoffs, the adoption of the more stringent ≤11 cutoff may inappropriately increase case detection of older persons who are otherwise not at elevated risk of adverse outcomes.
Thus, we conducted an exploratory study to determine the diagnostic performance and optimal cutoffs of the SPPB for clinically meaningful outcomes (functional ability, social activity, frailty, and gait speed) in an at-risk population of older adults attending a fall clinic compared to healthy controls. This was a secondary analysis using data from two earlier studies: the eSPPB kiosk validation study involving predominantly pre-frail patients attending a tertiary falls clinic (n=37),4) and healthy community-dwelling older persons from the “Longitudinal Assessment of Biomarkers for Characterization of Early Sarcopenia and Predicting Frailty and Functional Decline in Community-dwelling Asian Older Adults” (GeriLABS) longitudinal cohort study (n=200).9) We excluded participants with incomplete SPPB data or those who did not consent to the use of their data for future studies. Thus, our final sample comprised 165 community-dwelling older adults from the Falls Clinic (n=27; 73% of the original study) and the GeriLABS study (n=138; 69% of the original study). We used pre-specified validated cutoffs of clinical outcome measures which are associated with adverse outcomes, namely, the Lawton instrumental activities of daily living (IADL) <21,10) Frenchay Activities Index (FAI) <31,11) pre-frailty/frailty defined by FRAIL scale >0,9) and gait speed <0.8 m/s.12) Using receiver operating characteristic (ROC) curves generated for different outcomes, we determined the optimal cutoff values using the Youden Index and corresponding AUC. Based on the ROC cutoffs, we performed crosstabulation to derive the corresponding values for sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV), from which we determined the optimal cutoff for the SPPB. Statistical analyses were performed using IBM SPSS Statistics for Windows, version 28.0 (IBM Corp., Armonk, NY, USA). All statistical tests were two-tailed, and the level of statistical significance was set at 5%.
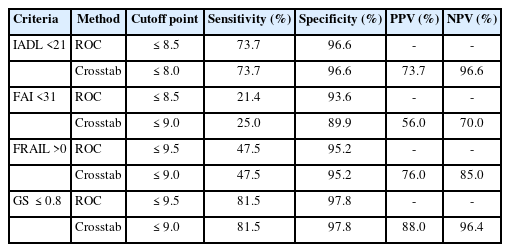
The GeriLABS cohort was younger (mean age: 67.3±7.3 vs. 77.1±6.9 years), more robust (mean FRAIL score: 0.17±0.45 vs. 1.2±0.83), and had a higher mean SPPB score (11.6±0.79 vs. 7.0±3.2, p<0.001) compared to the Falls Clinic group. The SPPB showed excellent discriminatory performance for reduced functional ability (IADL <21: AUC=0.872, 95% confidence interval [CI] 0.757–0.986), and the optimal SPPB cutoff of ≤8 yielded a sensitivity of 73.7% and a specificity of 96.6%. The SPPB showed fair performance for social activity (FAI <31: AUC=0.586, 95% CI 0.491–0.680) with an optimal cutoff score of ≤9 (sensitivity of 25.0%, specificity of 89.9%, PPV of 56%, NPV of 70%). Regarding the assessment of pre-frailty/frailty, the SPPB showed good discriminatory performance (FRAIL >0: AUC=0.762, 95% CI 0.664–0.860) using an optimal cutoff score ≤9 (sensitivity of 47.5%, specificity of 95.2%, PPV of 76%, NPV of 85%). Finally, the SPPB showed excellent performance for gait speed <0.8 m/s (AUC=0.972, 95% CI 0.945–0.998) for an optimal cutoff score of ≤9 (sensitivity of 81.5%, specificity of 97.8%, PPV of 88%, NPV of 96.4%) (Table 1).
The excellent discriminatory performance for functional ability, pre-frailty/frailty, and gait speed in our exploratory study supports the utility of the SPPB for assessing physical frailty and sarcopenia in at-risk community-dwelling older persons. Social activity is a complex phenomenon attributable to personal, social, and environmental factors beyond lower limb physical performance, which may explain the comparatively lower diagnostic performance of FAI in our study. Although the sensitivity range of the SPPB is quite broad (from 21.4% to 81.5%), it is highly specific (93.6%–97.8%). Our findings are similar to those of the Yishun Study, wherein the SPPB showed poor-to-moderate sensitivity but was highly specific for assessing sarcopenia.13) Thus, while the SPPB has overall good diagnostic performance for frailty and sarcopenia in at-risk community-dwelling older adults, it is better at “ruling in” true-positive cases than ruling out false-negative cases in the screening process. While an earlier Australian study reported that the SPPB has high sensitivity but low specificity with moderate (AUC=0.644–0.770) value in diagnosing sarcopenia, this was in the context of a lower cutoff (≤8) for the assessment of severe sarcopenia.14)
The optimal SPPB cutoff for clinically meaningful outcomes such as social activity and functional ability for identification of community-dwelling older persons at risk of sarcopenia and physical frailty for older adults in Singapore is ≤9, which is consistent with the AWGS-2019 recommendation and lower than the ≤11 cutoff in the Yishun Study. The participants in the Yishun Study were younger and more robust, whereas our study included predominantly pre-frail, at-risk patients from a fall clinic. Because ROC-derived cutoff points may not account for spectrum bias,15) this further supports the idea that reference values should be selected based on specific settings and patient characteristics. Adopting an appropriate cutoff score for the SPPB, which is predictive of clinically meaningful outcomes, can avoid overdiagnosis and unnecessary use of resources while fulfilling the purpose of identifying patients who would benefit from early intervention.8)
Taken together, the results of this study demonstrate that SPPB cutoff values should consider population characteristics and clinically meaningful outcomes. In at-risk older adults, an SPPB cutoff score of ≤9 yielded good diagnostic performance for the assessment of frailty, despite low-to-moderate sensitivity for social activity and pre-frailty/frailty. Owing to the small sample size of our exploratory study of at-risk compared to healthy older adults, further studies with larger sample sizes that examine the predictive validity of SPPB cutoffs for longitudinal adverse outcomes are needed to corroborate our findings.
Notes
CONFLICT OF INTEREST
The authors claim no conflicts of interest.
FUNDING
None.
AUTHOR CONTRIBUTIONS
Conceptualization, HHCH, DZY, JK, NHI, WSL; Data curation, HHCH, DZY, CNT; Investigation, HHCH, DZY, JK, NHI, WSL; Methodology, HHCH, DZY, JK, NHI, WSL; Project administration, CNT; Supervision, WSL; Writing-original draft, HHCH; Writing-review & editing, HHCH, DZY, NHI, WSL.